Why We Exist:
2010 saw the advent of The Knee Clinic; Alberta’s ONLY private knee clinic. In response to overwhelming public need for timely, accurate assessment, diagnosis and intervention of knee injuries, we offered a much-needed alternative to the public system. Fast forward to present day and wait times, not only in Alberta but indeed across the country have skyrocketed. Combine this increased wait time with an aging population, and knee issues are a bigger societal burden than ever. Our Knee Clinic is uniquely positioned to offer a broad spectrum of options for management of your knee, not limiting you to only medications and / or surgery.
We ascribe to three pillars in our approach to care.
1. The first pillar is to treat the actual problem.
In these modern times, it is insufficient to guess or approximate, when specialized clinical skill and access to advanced imaging modalities can allow us to be precise in our diagnoses. Our doctors take the time to investigate your issue in as much detail as required to ensure that we have the diagnosis pinpointed.
2. Once the specific diagnosis is established, we can move onto the second pillar which is to strengthen the area.
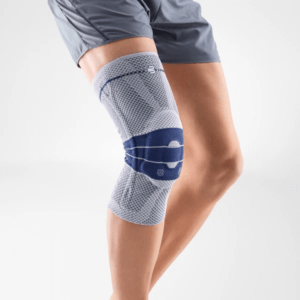
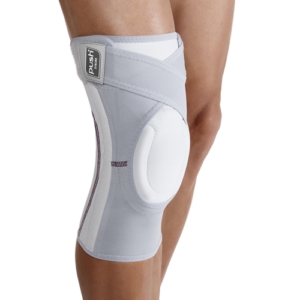
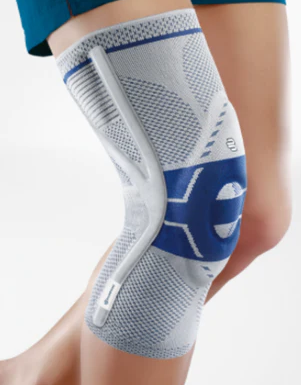
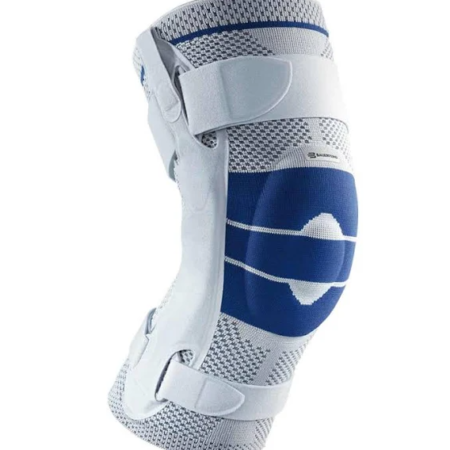
The knee is a unique joint with a vast range of competing responsibilities; It has to be very flexible, yet able to move quickly through a large range of motion. It has to be incredibly strong, allowing us to lift ourselves any additional weight that we’re carrying. Lastly, it has to be stable, despite being designed in a way that is inherently unstable.
3. The third and final pillar in our approach to care is to avoid or modify offending activities.
This involves continual patient education throughout the clinical journey as well as close attention to areas directly and indirectly related to the knee. This includes but is not limited to foot and ankle mechanics, lateral pelvic strength, appropriate footwear and even dietary, lifestyle and other potential inflammatory factors.
Canada’s First Online Knee Clinic
Prior to 2020, patients would travel to our clinic from all across the country and indeed from all across North America. Now in a changed world we are grateful to be able to reach out to our patients through online clinical consultations. You can book an online consultation online or by phone and your clinic directly at 403-457-5633.